
Suggested citation: European Centre for Disease Prevention and Control. Surveillance of COVID-19 in long-term
care facilities in the EU/EEA, 19 May 2020. Stockholm: ECDC; 2020.
© European Centre for Disease Prevention and Control, Stockholm, 2020
Erratum: on 9 June 2020 figures were corrected for Portugal in Annex Tables A1 and A2 at the request of
Portugal’s Ministry of Health.
TECHNICAL REPORT
Surveillance of COVID-19 at long-
term care facilities in the EU/EEA
19 May 2020
Introduction
The high COVID-19 morbidity and mortality observed among residents in long-term care facilities (LTCF) in EU/EEA
countries poses a major challenge for disease prevention and control in such settings. Furthermore, the lack of
special surveillance systems and the differences in testing strategies and capacities among countries may have led
to a significant under-ascertainment and under-reporting of cases, contributing to a general underestimation of the
disease burden and mortality in LTCFs. One factor that may have contributed to the spread of COVID-19 within
and between LTCFs relates to staff working while infectious, including symptomatic, pre-symptomatic, and
asymptomatic cases. Other contributing factors may have been staff working in more than one facility, lack of
personal protective equipment (PPE), lack of training and testing and testing being limited to symptomatic
individuals. Limited testing may have played a disproportionate role in under-ascertaining cases among this
population. The high prevalence of neurological conditions such as dementia and neuropathic disorders among
LTCF residents may result in atypical COVID-19 clinical presentations or the absence of evident signs or symptoms
until the patients’ conditions deteriorate.
The implementation of local and national monitoring systems for COVID-19 and other respiratory viruses in LTCFs
would help to identify outbreaks earlier, thus decreasing the spread within and between facilities. Early
identification of possible cases, rapid initiation of testing, and notification to the relevant health authorities so that
they can perform contact tracing, are key elements to reducing the size of COVID-19 outbreaks. A system should
be in place to screen residents daily for symptoms and to periodically test them, even in the absence of symptoms.
A graduated approach to testing is suggested, taking into account whether the facility is located in an affected or
unaffected area. It is also suggested that staff should be tested regularly (e.g. each week), with at least all
possible cases among residents being tested as soon as possible. If a confirmed case is identified in a resident or a
member of staff, comprehensive testing is recommended to identify asymptomatic cases and control measures
should be implemented immediately. Case data and infection prevention and control measures should be collected
at the facility. Facility-based data on cases in residents and staff and deaths in residents should be reported on a
daily basis at local, regional, national and EU/EEA level. An electronic reporting system is proposed to keep the
workload to a minimum. The best approach is a national, comprehensive and mandatory LTCF-based surveillance
system with cumulative daily or weekly reporting of possible, probable and confirmed cases among residents and
staff. However, reporting could also be based on a sentinel system as well as using public LTCFs, before recruiting
private and/or social sector LTCFs in a phased approach. Data collection should be conducted on a daily basis at
the facility, whilst reporting at local and national level should depend on the epidemiological situation in the area
and at the facility. For example, once confirmed COVID-19 cases are detected, reporting to local authorities should
be on a daily basis. Reporting at national level will provide data to assess the overall burden on LTCF residents,
and the geographic distribution of cases in LTCFs over time. Electronic reporting tools are the best option as a

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
2
complementary system to mandatory outbreak or confirmed case-based notification reporting since they offer easy
data collection and reduce the additional workload for limited staff in LTCFs.
Early and stringent isolation and protective measures implemented during outbreaks in similar settings have shown that
protective effects can reduce the spread [1]. Prevention and control of respiratory disease outbreaks in LTCFs requires a
multi-faceted approach, including non-pharmaceutical countermeasures (e.g. use of face masks, cohorting and isolation
of infected people). Training of personnel and provision of information on how to adhere to hygiene recommendations is
crucial, especially in the context of COVID-19, prior to the identification of possible, probable, or confirmed cases.
It is of paramount importance to be able to rapidly identify, assess and control COVID-19 outbreaks in LTCFs in
order to protect this particularly fragile population. This document provides guidance for EU/EEA Member States
planning to implement monitoring systems at LTCFs and describes the surveillance objectives.
Consulted experts
External experts: Siri Hauge (Norwegian Public Health Institute), Lisa Domegan and Joan O’Donnell (Health Service
Executive-Health Protection Surveillance Centre Ireland); Sibylle Bernard-Stoecklin and Kostas Danis (Santé
Publique France); Katrien Latour (Sciensano, Belgium); Enrico Ricchizzi (Regional Health and Social Agency - Emilia
Romagna, Italy); Brigitta Schweickert, Nicole Schmidt, Muna Abu Sin and Tim Eckmanns (Robert Koch-Institute,
Germany); José-Artur Paiva (PPCIRA – DGS, Portugal);
All external experts are nationally nominated National Focal Points or Operational Contact Points for Healthcare-
associated Infections or Influenza.
ECDC experts: Cornelia Adlhoch, Bruno Cianco, Pete Kinross, Angeliki Melidou, Gianfranco Spiteri, Carl Suetens
WHO Regional Office for Europe expert: Pernille Jørgensen.
EU OSHA (European Agency for Safety and Health at Work) expert: Elke Schneider
Public health issue and objective
Residents in LTCFs are a vulnerable population group. They are often old and frail, with complex health needs,
underlying chronic diseases and immunosenescence, commonly relying on medical support. People aged 65 years
and above, especially those with underlying co-morbidities, are disproportionately affected by adverse outcomes of
COVID-19 compared to younger age groups [2].
The closed environment of LTCFs facilitates the spread of infectious diseases among residents. Other respiratory
infections, such as influenza, also cause outbreaks in LTCFs with substantial morbidity and high mortality. A large
number of COVID-19 outbreaks have been reported in European LTCFs to date [3]. Other specialist types of LTCF,
such as those for physical rehabilitation or for persons with physical, mental, intellectual or sensory disabilities, are
environments where a relatively large number of people congregate, and are consequently prone to infectious
disease outbreaks, even though the mean age of these residents tends to be lower.
This document aims to provide guidance to Member States for the development of COVID-19 surveillance at
LTCFs. The surveillance objectives are outlined in the document. Collection of individual case data within facilities
for local use, as well as facility-based data to be shared with local and national authorities, will provide the
opportunity for early intervention. It will help to assess and prevent spread within and across facilities, reduce the
overall size of COVID-19 outbreaks, and minimise impact of the diseases, both among residents and staff
members. These data will also help at national and international level to provide insight into changes in the
geographical distribution over time, and the overall impact of the COVID-19 within this risk group.
This document builds on guidance previously published by WHO:
Prevention and control of outbreaks of seasonal
influenza in long-term care facilities: a review of the evidence and best-practice guidance and ECDC: Infection
prevention and control and preparedness for COVID-19 in healthcare settings - second update.
Target audience
The target audience for this guidance is public health experts, healthcare professionals and administrators working
in long-term care facilities at local/regional level, and national public health authorities.
Background
On 31 December 2019, a cluster of pneumonia cases of unknown aetiology was reported in Wuhan, Hubei
Province, China. On 9 January 2020, China CDC reported a novel coronavirus as the causative agent of this
outbreak, coronavirus disease 2019 (COVID-19). Case-based data collected by ECDC from EU/EEA countries
through The European Surveillance System (TESSy) has shown increasing rates of hospitalisation for reported
laboratory-confirmed cases over 50 years of age. These rates were highest in the age-group 65 years and above
[2]. The risk of severe infection in the elderly is also evident in case fatality data from TESSy (44% of all deaths
were in those aged 65–79 years and 46% were in those aged 80 years and above.)

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
3
COVID-19 in long-term care facilities
A high proportion of LTCFs across Europe and globally have reported COVID-19 outbreaks, with high rates of
morbidity and case fatality in residents and high rates of staff absenteeism [4-6]. The transmission dynamics of
COVID-19 combined with low availability of testing have fuelled a rapid spread within and between facilities,
leading to high morbidity and mortality among residents in these settings.
At a skilled
1
nursing facility in King County, Washington State (US), within 23 days of a first SARS-CoV-2 positive
test result, 64% (n=57/89) of LTCF residents had tested positive. The facility performed two comprehensive point
prevalence surveys (PPS) in 76 residents, one week apart. In the first PPS, one third of the LTCF residents (21/76;
28%) tested positive for SARS-CoV-2 and had symptoms, while one third (27/76; 36%) tested positive but had no
symptoms. However, within seven days, 24/27 (89%) ‘asymptomatic’ cases had developed compatible symptoms
(i.e. they had been pre-symptomatic.) As of 3 April 2020, 15/57 (26%) of the SARS-CoV-2-positive residents at this
facility had died [7]. This underlines the importance of taking measures for those without symptoms at facilities
with cases [8]. In Belgium, as of 5 May, systematic testing of all residents and staff in a selection of LTCFs with
confirmed cases identified that 73% (5 695/7 751) of PCR-positive cases were asymptomatic [9].
Under-ascertainment and under-reporting of COVID-19 cases in LTCFs has been a common feature of the COVID-
19 surveillance in Europe. The increasing number of reported outbreaks, which have been associated with high
mortality, indicates the requirement for a targeted approach to the protection of vulnerable groups in such
settings. The majority of European countries did not have surveillance systems for LTCFs in place before the
current pandemic – i.e. systems able to systematically and consistently monitor respiratory diseases and provide
timely reporting at local or national level to inform interventions. In recent weeks, local, regional or national
monitoring systems have been updated or created to include LTCFs. Example systems that can report COVID-19
cases are listed at the end of this document (see Annex). In some EU countries, the proportion of COVID-19 cases
in LTCFs who have died has exceeded 60% of all reported deaths, underlining the severe impact of COVID-19 on
this frail population [4].
In Belgium, as of 17 May 2020, 51% of the 9 052 COVID-19 related fatal cases were reported from LTCFs, with only
23% of cases laboratory-confirmed [9]. Systematic testing for SARS-CoV-2 among all LTCF residents revealed that 4%
(5 640/141 089) were positive and more commonly symptomatic than asymptomatic (25% and 3%, respectively). Tests
were also performed among LTCF staff, with 3 106/136 282 (2%) testing positive. The overall test positivity is higher in
symptomatic than asymptomatic staff (11% and 2%, respectively). However, the overall number of asymptomatic cases
among residents and staff was 75% (6 540/8 746) of all cases that tested positive at these facilities.
France has established a dedicated notification system for COVID-19 cases reported by LTCFs. Between 1 March and
11 May 2020, 7 469 facilities reported cases, of which 4 367 (66%) were in nursing homes for the elderly and 2 245
(34%) were at other LTCFs, such as facilities for disabled persons or children and young adults. Of the 73 435
reported confirmed and probable cases among residents, 13 539 (17%) died, 3 321 in hospitals and 9 501 at the
facilities, which represent 50% of all deaths
[10]. In addition, 39 294 cases were reported among staff members.
As of 17 May 2020, Germany had reported 22 071 infections related to institutions caring for elderly (long-term
care, nursing homes), disabled people, homeless people, migrants, or those in prisons. Of these, 8 536 cases were
in staff (42 died) and 14 740 cases were in residents. Of the residents 2 966 died (20%), representing 37% of all
7 914 deaths related to COVID-19 in Germany [11].
Ireland has a dedicated outbreak reporting surveillance system for all infectious diseases, which is currently being
used for COVID-19. As of 9 May, 418 COVID-19 outbreaks had been notified in residential facilities (including
nursing homes for the elderly, direct provision centres and prisons) in Ireland, with 5 698 laboratory confirmed
cases and 727 deaths in confirmed cases linked to these outbreaks [12].
In Norway, 136 (61%) of all 224 fatal cases reported by 11 May 2020 were in ‘home care’ or ‘other health
institutions’ [13].
In Spain, as of 11 May, 17 730 fatalities have been reported from 5 400 affected care-home residents,
representing 66% of all fatal cases linked to COVID-19 [14].
In Sweden 212 of 400 LTCFs in the Stockholm region have reported 1 711 COVID-19 cases, representing 630 (45%) of
1 406 deaths in Stockholm [15-18]. In Stockholm county, 400 LTCFs participated in a survey during the period 12–15
April 2020, with 212 (53%) reporting that they had had confirmed COVID-19 cases. Of these 212 LTCFs, 123 indicated
the size of their outbreaks, with 37% reporting 4–10 cases, and 22% reporting >10 cases. Across Sweden, 541 care
homes have been affected and 2 866 confirmed COVID-19 cases with 948 deaths have been reported from LTCF
residents aged over 70 years, representing 50% of all COVID-19 related deaths in this age group [19]
In the United Kingdom, the Office for National Statistics lists 6 997 (21%) deaths in care homes as COVID-19-
related out of a total 33 337 registered COVID-19 deaths in England and 404 (25%) deaths in care homes out of a
total of 1 641 COVID-19 deaths in Wales between 28 December 2019 and 1 May/9 May 2020 [20]. The Care
1
US healthcare institution that meets federal criteria for Medicaid and Medicare. For more details see
https://www.skillednursingfacilities.org/resources/what-are-skilled-nursing-facilities-/

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
4
Quality Commission lists 8 314 deaths in care homes involving COVID-19 as having been notified between 10 April
and 8 May 2020 in England and 350 deaths in care homes in Wales [20,21].
As of 17 May, Scotland reported that 632 (58%) of care homes for adults had reported at least one suspected case
and 463 more than one case of COVID-19, with 5 096 suspected cases in total [22]. Up to 10 May, 1 438 deaths
involving COVID-19 had been reported from care homes, representing 45% of all 3 213 deaths [23].
A similar situation has been reported from North America, including both Canada and the United States (US), with
more than 10 000 deaths reported to be linked to LTCFs in the US as of 23 April 2020 [24-26]. By 14 May more than
7 000 facilities in 41 States across the US had reported being affected, with over 150 000 COVID-19 cases, including
more than 30 000 deaths [27]. In the US, the first COVID-19 outbreak in a skilled nursing facility was notified on 28
February 2020 in King County, Washington. By 18 March, 167 cases had been identified among residents, personnel
and visitors. The hospitalisation rate among residents and staff was 50% and the case fatality rate among residents
was 34% [28,29]. Within a few weeks, another 30 skilled nursing and assisted living facilities in the King County had
also reported COVID-19 outbreaks. The investigation revealed that movement of healthcare personnel among
different facilities contributed to the spread of the virus across the County to other LTCFs. In King County, the
diagnostic investigations included testing of asymptomatic residents and staff to evaluate the spread within facilities.
Identification of asymptomatic infections in a facility resulted in the implementation of a control strategy for the
facility as a whole and isolation of all residents, rather than just isolating symptomatic persons [30]. Focussing
interventions at LTCFs on symptomatic cases and staff is unlikely to be sufficient to control transmission, as half the
cases or more may be asymptomatic [7,9].
European long-term care facilities (LTCF)
LTCFs encompass a broad range of institution types, from those that are purposefully home-like to those providing
specialised medical care [31]. Although most LTCFs are for older people, some are for persons with physical,
mental, intellectual or sensory disabilities, while others are palliative care centres and rehabilitation centres [32].
ECDC’s definition of an LTCF is provided below. ECDC estimates that in 2016–2017 there were 64 471 nursing
homes, rehabilitation centres and mixed LTCFs in EU/EEA countries, representing a total of 3 440 071 beds (see
Annex, Table A1 and Table A2).
In the third ECDC point prevalence survey of healthcare-associated infections and antimicrobial use in European
LTCFs, 2016–2017 (HALT-3), 3 052 LTCFs participated from 24 EU/EEA countries, North Macedonia and the
Republic of Serbia. Data from these LTCFs were analysed for a sample of 1 797 nursing homes, residential homes
and mixed facilities. Only 25% of the participating EU/EEA LTCFs had a coordinating physician at their facility,
while 48% had external medical coordination and 4.5% had both. Overall, 39.1% of all LTCFs had an infection
prevention and control (IPC) committee in place, which had met 3.8 times during the previous year on average.
However, there were large differences between countries, with no LTCFs having such committees in Greece and
Slovakia, and all participating LTCFs in Croatia having them. The majority of LTCFs (71.0%) had at least one
person with IPC training at their disposal. These persons were either a nurse (50.2%), a doctor (5.3%), or a team
of both (44.5%). They were most commonly based within the reporting LTCF (43.0%), while a sizable minority
were based externally (32.9%), or worked both internally and externally (24.1%). These data are likely to be an
overestimate of the EU/EEA situation, as they are from LTCFs that were able to participate in this voluntary survey.
Definitions
Long-term care facilities
Long-term care facilities (LTCFs) include institutions such as nursing homes, skilled nursing facilities, retirement
homes, assisted-living facilities, residential care homes or other facilities. These facilities take care of people
requiring support who find it difficult to live independently in the community due to the interaction between
barriers in the environment and physical, mental, intellectual or sensory impairments possibly as a result of old
age, or chronic medical conditions. LTCFs for all age-groups are included.
LTCFs typically have residents who:
• need constant supervision (24 hours a day)
• need ‘high-skilled nursing care’ (i.e. more than ‘basic’ nursing care and assistance for daily living activities)
• are medically stable and do not need constant ‘specialised medical care’ (i.e. care administered by
specialised physicians)
• do not need invasive medical procedures (e.g. ventilation).
For the point prevalence surveys of European LTCFs in 2010, 2013 and 2016–2017, ECDC’s definition of an LTCF
excluded certain facility types [31]. These were hospital long-term care wards, hostel care (hostel without any type
of nursing care), sheltered care houses, day centres, home-based centres and protected living. However, given
that these facility types also constitute an environment susceptible to COVID-19 outbreaks in vulnerable people,
countries may wish to consider instituting COVID-19 surveillance in these settings too.

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
5
Definition of LTCF types
General nursing homes
In these facilities, residents need medical or skilled nursing and supervision 24 hours
a day. These facilities principally
provide care to seniors with severe illnesses or
injuries.
Residential homes
In these facilities residents do not have access to the services and support in the
community to be able to live independently. They require supervision and assistance
in order to go about their daily lives.
These facilities usually include personal care,
housekeeping and three meals a day.
Specialised LTCFs
These facilities are specialised in one specific type of care (e.g. physical impairment,
chronic diseases such as multiple sclerosis, dementia, psychiatric illnesses,
rehabilitation care, palliative care or intensive care.)
Mixed LTCFs
These facilities provide different types of care at the same facility (a mix of the
above-mentioned LTCF types).
Other LTCFs
Other facilities which cannot be classified among the LTCF types above.
Note: This classification does not imply that the characteristics of residents within each facility type are strictly homogeneous.
Case definition
The case definition for EU surveillance is available on ECDC webpage. A modified case classification for testing and
reporting from LTCFs can be found in Table 1. The clinical presentation of COVID-19 below outlines additional
clinical symptoms compatible with COVID-19 that should be considered for the identification of a possible case in
LTCF residents.
Table 1. Suggested case classification
Possible case
Any person meeting the clinical criteria - at least one of the following symptoms
2
:
• cough
• fever
• shortness of breath
•
sudden onset of anosmia, ageusia or dysgeusia
Probable case
Any person meeting the clinical criteria (see possible case) with an epidemiological link:
• close contact
3
with a confirmed COVID-19 case in the 14 days prior to onset of symptoms;
• having been a resident or member of staff, in the 14 days prior to onset of symptoms, in a residential
institution for vulnerable people where ongoing COVID-19 transmission has been confirmed;
OR
Any person meeting the diagnostic criteria:
•
radiological evidence showing lesions compatible with COVID-19
Confirmed case
Any person meeting the laboratory criteria:
• detection of SARS-CoV-2 nucleic acid in a clinical specimen
4
.
COVID-19-related mortality definition
Mortality monitoring [33]: a COVID-19 death is defined for surveillance purposes as a death resulting from a
clinically compatible illness in a probable or confirmed COVID-19 case, unless there is a clear alternative cause
of death that cannot be related to COVID disease (e.g. trauma). There should be no period of complete recovery
between the illness and death. A death due to COVID-19 may not be attributed to another disease (e.g. cancer)
and should be counted independently of pre-existing conditions that are suspected of triggering a severe course of
COVID-19.
Existing national surveillance systems may not be able to apply this case definition fully. For example, France does
not exclude fatal cases based on alternate causes of death, or a period of recovery between illness and death.
Rather, France records all in-hospital and in-LTCF deaths in LTCF residents who were probable or confirmed
COVID-19 cases.
2
Additional less specific symptoms may include headache, chills, sore throat, muscle pain, fatigue, vomiting and/or diarrhoea.
3
Close contact defined according to the ECDC guidance document ‘Contact tracing: Public health management of persons,
including healthcare workers, having had contact with COVID-19 cases in the European Union’
4
For further guidance on laboratory issues, see https://www.ecdc.europa.eu/en/novel-coronavirus/laboratory-support

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
6
Approaches to monitoring COVID-19 in long-
term care facilities
Surveillance objectives
The objectives of COVID-19 surveillance in LTCFs at local, regional and national level, as well as EU/EEA level, are
as follows:
• detect COVID-19 infections in LTCF residents and staff, to enable appropriate implementation of infection
prevention measures to limit the size of outbreaks (local objective);
• monitor the total number and proportion of affected LTCFs, to provide situational awareness;
• monitor changes in the intensity and geographical distribution of affected LTCFs with time, to assess
prevention and control efforts;
• monitor the impact and severity of COVID-19 in LTCFs, including impact on overall mortality in LTCF
residents, in order to provide situational awareness of the current burden of disease and to inform
mitigation measures.
See also ECDC surveillance strategy
.
To acquire nationwide situational awareness of the current and expected burden of COVID-19 in LTCFs, EU/EEA
countries may consider implementing a national comprehensive LTCF-based surveillance system with cumulative
daily or weekly reporting of possible, probable and confirmed cases in residents and staff. However, countries that
seek to obtain comprehensive national coverage may require a phased approach to implementation, due to the
fact that long-term care services are provided by a mix of public sector, private sector and social sector (e.g. non-
profit, non-governmental) institutions. In such countries, approaches might include:
• a voluntary system that does not aim for national representativeness, such as a convenience sample,
potentially with sub-national coverage at the start;
• a sentinel system, based on country-wide selection of facilities, to serve as indicators for their respective region;
• initially prioritising participation of public LTCFs, before recruiting private and/or social sector LTCFs in a
phased approach.
Syndromic surveillance
The key to preventing and controlling outbreaks is systematic monitoring of all residents and staff at an LTCF.
Residents should be monitored for the symptoms set out below by measuring temperature, oxygen saturation via
pulse oximetry, and respiratory rate at least once a day, or once every shift to early identify possible cases and
initiate testing. Decreased oxygen saturation (<95%) and increased respiratory rate (>25/min) can be indicators
measured directly at the resident’s bedside.
LTCFs should update their administrative records daily on the basis of syndromic surveillance, to record whether a
resident has received a COVID-19 test, been isolated due to COVID-compatible symptoms, and/or required any
other non-standard IPC measures.
Clinical presentation of COVID-19
COVID-19-compatible symptoms include influenza like-illness (ILI: sudden onset of symptoms and at least one of
the following four systemic symptoms: fever or feverishness, malaise, headache, myalgia and at least one of the
following three respiratory symptoms: cough, sore throat or shortness of breath) or acute respiratory infection
(ARI: sudden onset of symptoms, and at least one of the following four respiratory symptoms: cough, sore throat,
shortness of breath or coryza), can be used to identify symptomatic cases.
However, it is important to note that the clinical presentation of disease may be very mild or atypical, or involve
unexplained deterioration of health. In addition, outbreak investigations in LTCF have identified a high proportion
(around 15%) of asymptomatic confirmed cases. Other atypical presentations in older adults and people with
underlying conditions include anorexia, anosmia, apathy, conjunctivitis, diarrhoea, disorientation, lethargy, loss of
weight, nausea, rash, respiratory distress, somnolence, stuffed nose or vomiting [34,35].
Testing approach
Laboratory testing of possible cases should be initiated together with COVID-19 surveillance in accordance with
Table 2. Given the rapid spread at LTCFs with attack rates of 50% or above and the severe outcomes among LTCF
residents, the following approach should be considered:
• single possible cases with clinical symptoms compatible with COVID-19 should be isolated and tested as
soon as possible, with laboratories prioritising such specimens with or without an epi link to COVID-19;

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
7
• when a first case is confirmed in a resident or staff member of an LTCF, a comprehensive testing strategy
of all residents and staff should be strongly considered, including those without symptoms;
• if confirmed cases have been observed in the LTCF, post-mortem testing of deceased residents could be
considered.
The policy has to be adapted to local capacity and the epidemiological situation in the community. Local health
authorities need to be informed when a possible case is identified. The early identification of asymptomatic or
atypical and mild cases should initiate comprehensive testing to support control efforts and allow outbreak
response measures, to cohort residents accordingly. Widespread testing can also guide infection control, isolation
and early clinical care to minimise severe disease and fatal outcomes.
Regular testing of all staff could be considered, in particular in areas with community transmission. As a minimum,
symptomatic staff, including those with mild symptoms, should be prioritised for testing in order to guide decisions
on exclusion from work. Current ECDC guidance recommends that staff with symptoms compatible with COVID-19
should not come to work and should inform a designated person at the LTCF:
Infection prevention and control and
preparedness for COVID-19 in healthcare settings. Staff should be tested at regular intervals (e.g. weekly or bi-
weekly), depending on the availability of resources, to exclude the possibility of asymptomatic infection and limit
the introduction of COVID-19 at the facility.
If visitors are allowed to enter the facilities, depending on the epidemiological situation in the area where the
facility is located, they should wear facemasks, and keep a physical distance of 2 metres as well as adhering to
strict hygiene measures. Regular visitors should also be considered for testing if it is available. Visitors with
symptoms of respiratory infections should not visit the facility.
If staff or visitors are found to be positive, isolation and contact tracing should be applied as advised in the IPC
guidance: Infection prevention and control and preparedness for COVID-19 in healthcare settings
. All facilities
where staff have tested positive need to be included in the immediate measures implemented by the local health
authorities and comprehensive testing also needs to be carried out at these facilities.
ECDC has published guidance for discharge and ending isolation in the context of widespread community
transmission of COVID-19.
Table 2. Testing recommendations for LTCFs, based on different scenarios
Measure/scenario
Laboratory testing of
residents
Laboratory testing of staff
Reporting to local
authorities
No cases
Affected area:
random samples, dependent on
testing capacities*
Unaffected area:
dependent on national testing
policy for LTCFs.
Affected area:
consider comprehensive testing
for all staff weekly/biweekly*
Unaffected area:
dependent on national testing
policy for LTCFs or random
samples.
Affected area: weekly or
monthly.
Unaffected area: monthly
≥1 possible case
As soon as possible, test at
least all possible case(s)*.
As soon as possible, test all
possible case(s)*, optimal:
comprehensive for all staff.
Affected area: daily
Unaffected area: weekly.
Sudden increase in
possible cases: daily.
≥1 confirmed case
Comprehensive testing of all
residents including those who
have died, dependent on
testing capacity*.
Comprehensive testing for all
staff, test regularly (weekly-bi-
weekly) if possible.
Daily
Affected area: ongoing or presumed ongoing community transmission; according to definition in The European Surveillance System (TESSy).
Reporting protocol: see ECDC webpage: https://www.ecdc.europa.eu/en/covid-19/surveillance
.
Testing and reporting schemes should be in line with national recommendations for LTCFs and dependent on the epidemiological situation in the
country and region and should include testing of asymptomatic residents and staff.
* if testing capacity is limited, consider random testing or a pooling of samples https://jamanetwork.com/journals/jama/fullarticle/2764364
Sample collection and testing method
Ideally, clinical samples should be collected on site at the LTCF, with the support of the local public health
authority. More information is available here
. Validated self-swabbing kits may be considered. Respiratory
diagnostic specimens (nasopharyngeal swab, oropharyngeal (throat) swab, nasopharyngeal aspirate or nasal wash)
should be collected as soon as possible after symptom onset from every person presenting with symptoms.
Arrangements for specimen collection and transport should be established proactively with local
microbiology/virology laboratories. Currently, the preferred method of viral diagnosis is RT-PCR, performed by
specialised laboratories designated by local/national authorities.
TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
8
Laboratory diagnostics should focus on SARS-CoV-2 and include influenza (including the determination of the viral
type and subtype) when influenza is circulating. For further information see ECDC surveillance strategy
and WHO’s
Laboratory testing for coronavirus disease 2019 (COVID-19) in suspected human cases: Interim guidance.
Data collection and reporting
Data collectors and reporters
LTCF management should appoint named staff members who are responsible for daily active monitoring of the
occurrence of symptoms/signs of COVID-19 in all residents and staff at the facilities and for reporting these to
relevant local/national authorities, depending on the case definition. Staff should be trained to identify and assess
the symptoms mentioned in the previous section on clinical symptoms.
Data collection
The following suggested time periods for daily, weekly or monthly reporting need to be adjusted by each country
depending on the respective epidemiological situation overall and the particular area, as well as the ability of the
facilities and health authorities to report. See suggestions in Figure 1 and Table 2. LTCFs should collect daily
records of the situation at the facility (line list: Table A3). At the beginning of the outbreak a report should be
made available by each facility to the local health authorities describing the characteristics of the facility and
detailing the number of residents and staff (Table A4). Following the confirmation of a case, reporting to the
respective local or regional health authorities should be carried out on a daily basis and the data to collect are
suggested in Table A5. Weekly or monthly reporting to the respective local or regional health authorities should be
continued even if no cases are identified (‘nil reporting’, Table A5). The ‘nil reporting’ on a weekly basis may
represent a high reporting burden and if feasible, this needs to be reassessed by the relevant authorities.
Figure 1. Reporting scheme
* If regional/national health authorities ask LTCFs to send reports to local health authorities.
Collection of data at the facility should be warranted year-round, but modified based on the epidemiological
situation. The observation of a possible case should be reported immediately to local health authorities and if
confirmed, daily reporting should be initiated. If a notably high rate of severe outcomes or case fatalities is
observed in an LTCF, an immediate alert should be sent to the local authority. Reporting should follow the same
procedures as for other outbreaks. Reporting from the LTCFs with ongoing outbreaks to local, regional and national
level should be conducted on a daily or, as a minimum, weekly basis.
Daily reporting should be maintained after symptoms come to an end in the last case, in order to confirm the end
of an outbreak. The duration of the continued daily reporting should be agreed with local/national authorities and
could last until 28 days after the last case to confirm the end of outbreaks (no new cases for 2x maximum
incubation period). Regular laboratory screening should be maintained, to monitor for reintroductions, as outlined
in Table 2.
Mandatory reporting of possible and confirmed cases to relevant health authorities should continue. Data from
LTCFs should be a separate and additional source of information about the situation in facilities regionally and
nationally. Electronic reporting through national online platforms is suggested as the most efficient option and an
electronic solution could also address the simultaneous fulfilment of mandatory reporting requirements of
possible/confirmed cases to avoid double work for staff. The development of an electronic reporting system is
crucial, but the delayed implementation or lack of such a system should not be an obstacle to initiating monitoring
at LTCFs.
ECDC
Local*, regional and national health authority
Voluntary: weekly or monthly
Long-term care facility
No cases
Affected area: weekly or monthly
Unaffected area: monthly
≥1 possible case
Affected area: daily
Unaffected area: weekly or monthly
≥1 confirmed case
daily

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
9
The suggested reporting forms (see Table A3, Table A4, Table A5, Table A6) could be supplemented by further
information enabling informed guesses to be made about the situation in LTCFs or providing an update on the
implementation status of recommendations to prevent and manage COVID-19 in LTCFs. Core variables could be
labelled mandatory or optional, depending on the individual regional or national situation, in the reporting form.
Draft data reporting forms for this purpose and a simple standalone MS Excel file (with look-up lists to standardise
data entry) are provided in the annex and available on the webpage.
Data to be collected at the facility
Each LTCF should maintain a table in an overview document that provides the information listed below for each
day of an outbreak and for each patient (line list, a sample Excel sheet is shown in Table A3).
Other items to consider including are resident details such as room number, floor, etc. This line list containing
individual patient data should remain at the facility.
The assigned LTCF reporting team should also maintain additional records, to enable local health authorities to
perform any required outbreak investigations efficiently, in order to promptly determine actions to minimise the
severity/extent of that outbreak:
• description of the practices of staff and any visitors, including a record of the areas visited at the facility,
duration of attendance, and relevant activities’
• contact details of any visitor(s);
• layout of the LTCF;
• assignment of dedicated single rooms/floors for infected patients;
• environmental cleaning regimens, including waste disposal;
• existing IPC measures;
• presence/insufficient availability/unavailability of:
− masks (and their type), gowns, gloves, visors, and other relevant PPE
− appropriate environmental cleaning regimens, including waste disposal.
The minimum data to collect should be the total number of residents and staff during the previous seven days, and
number of possible, probable and confirmed of cases among them.
Data on work absenteeism might be helpful for the assessment but needs to comply with data protection
requirements. Collecting information on the number of days of staff absence due to respiratory symptoms, confirmed
COVID-19 disease or home isolation/quarantine after contact with a confirmed COVID-19 case is encouraged.
Data to be reported from LTCF to (local/regional/national) health authorities
Each LTCF should provide the following data on a daily or weekly basis (or monthly for unaffected areas) to local
authorities, which will then be passed to national authorities
. Data collection, testing and reporting should follow
the outline proposed in Table 1, depending on the epidemiological situation and national requirements.
During the first report when a first possible case is reported, each LTCF should specify its LTCF type (see definition
above) according to Table A4.
Each LTCF should provide data on a daily or weekly basis to local health authorities, depending on the
epidemiological situation and national requirements, as in Table A5, after at least one possible case has been
identified. This should continue on a daily basis once a COVID-19 case has been confirmed among LTCF residents
or staff. For countries that may not be able to distinguish between staff and residents in their surveillance data, we
suggest the option of reporting the total number for both residents/staff.
Data to be reported from local/regional to national health authorities
Each local health authority should report the same information weekly to (at least) the regional/national authorities
(depending on the healthcare and surveillance system structure in the respective country).
Reporting to ECDC
National authorities in EU/EEA countries are encouraged to consider sharing the above LTCF-level data with ECDC,
on a voluntary basis, with anonymised LTCF-level identifiers in each report.
These data will enable ECDC to provide countries with an assessment of the geographical extent of COVID-19 in
LTCFs, also in terms of the proportion of affected facilities, including changes over time, by country. Analysis of
multi-national LTCF-level data which includes LTCFs without cases may permit identification of LTCF characteristics
relevant to COVID prevention and control that were not apparent within single national datasets. LTCF-level data
will also enable the stratification of indicators, such as the incidence of possible/probable cases for LTCFs with and
without confirmed cases. The variable that indicates the geographical area of the LTCF should preferably be
NUTS2, or NUTS1, as community prevalence/incidence data are commonly available at this granularity.
The TESSy metadata will contain a new ‘record type’ for this LTCF dataset. Reporting of LTCF-based data should
be entered into this new record type. Reporting of the national case-based or aggregate reporting of probable and
confirmed COVID-19 cases to the record types ‘NCOV’ and ‘NCOVAGGR’ should continue separately (see TESSy
metadata). See ECDC related documents: https://www.ecdc.europa.eu/en/covid-19/surveillance
.

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
10
Data at local/regional and national level
Minimum data to be collected to fulfil surveillance objectives:
• applied prevention and control measures;
• total number and proportion of affected LTCFs regionally and nationally;
• changes in the distribution of affected LTCFs geographically over time;
• number and proportion of (possible,) probable and confirmed COVID-19 cases among residents;
• number and proportion of (possible,) probable and confirmed COVID-19 cases among staff;
• number and proportion of (possible,) probable and confirmed fatal cases of COVID-19 among residents;
• total number of all-cause deaths from LTCFs;
• identification of LTCF characteristics relevant to COVID prevention and control.
Infection prevention and control measures
Enhanced infection, prevention and control measures should be in place in all LTCFs. This includes separation of
possible cases with respiratory symptoms, even without laboratory confirmation. Respective IPC measures for
COVID-19 in healthcare facilities focus mainly on rapid identification, source control, administrative controls,
environmental measures and personal protective measures according to national or local authority guidelines.
ECDC has published guidance
that includes occupational health and safety requirements in healthcare settings and
LTCFs. In areas with sustained community transmission, in addition to strict hand hygiene, the wearing of surgical
masks or FFP2 respirators should be considered by all LTCF staff when caring for all residents. Other measures to
consider are temporary closure of LTCFs for visitors and systematic testing of all LTCF staff. For relevant literature
that includes LTCFs, please consult the following:
A systematic review on the causes of the transmission and
control measures of outbreaks in long-term care facilities: Back to basics of infection control.
ECDC has published the following documents relevant for this area:
Infection prevention and control and preparedness for COVID-19 in healthcare settings.
Guidance for disinfection of environments in healthcare and non-healthcare settings potentially contaminated with
SARS-CoV-2
Please also see WHO’s guidelines:
Infection Prevention and Control guidance for Long-Term Care Facilities in the context of COVID-19
Staff health and safety
The health and safety of staff working at LTCFs is paramount. Not only for their own protection but also to help
prevent the spread of the virus and to improve overall care. There is a comprehensive body of EU legislation to
protect workers' health and safety in the workplace. Additional measures that need to be taken when COVID-19
cases are registered at LTCFs may pose additional risks to staff in terms of higher physical and mental workload,
longer working hours and increased administrative workloads. Workplace risk assessments in accordance with
occupational safety and health legislation will therefore need to be revised and the occupational health and safety
measures adapted in agreement with occupational safety and health services and workers, taking into account all
types of risk (also taking into account the additional physical load when wearing personal protective equipment.)
Where there is a safety and health committee in place, it should be consulted.
Appropriate staffing of LTCFs should be reviewed to be able to perform patient care tasks, monitor oxygen
saturation and breathing frequency and measure the temperature of residents while also collecting data to be
reported to health authorities. Each country needs to find a way (e.g. IT solutions) to minimise the workload for
facilities while achieving a good cost-benefit ratio.
Non-binding guidelines developed at EU level aim to help employers and workers to stay safe and healthy in a
working environment that has changed significantly because of the COVID-19 pandemic. They give advice on risk
assessment and appropriate measures, such as minimising exposure, resuming work, coping with absences and
taking care of workers who have been ill. They also contain useful links to national guidance in specific sectors,
including health and care services. More information on occupational safety and health is available here:
Overview: https://osha.europa.eu/en/themes/covid-19-resources-workplace
COVID-19: guidance for the workplace: https://oshwiki.eu/wiki/COVID-19:_guidance_for_the_workplace
COVID-19: Back to the workplace - Adapting workplaces and protecting workers
https://osha.europa.eu/en/publications/covid-19-back-workplace-adapting-workplaces-and-protecting-workers/view
Other considerations and limitations
Seasonal influenza and pneumococcal vaccination, as well as other routine vaccines should be offered to residents
and staff in accordance with the national or regional recommendations. During the influenza season, prophylaxis
and treatment with neuraminidase inhibitors for influenza can be considered in accordance with national
recommendations.

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
11
Management of visitors to facilities and provision of face masks, introduction of IPC measures, etc. will possibly
add a substantial additional burden for staff and impact the time available for care tasks. Ethical considerations
regarding long-term isolation (and restriction of visits) to residents have to be balanced against the impact of the
infection on residents and staff.
Additional reporting requests for LTCFs, that may be already understaffed under normal circumstances outside of
the pandemic, will add an extra burden that might be difficult to fulfil without affecting basic patient care. In
addition, the skills required for electronic reporting might be challenging for some LTCFs, particularly if they usually
carry out paper-based reporting. These limitations need to be considered when implementing LTCF monitoring.

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
12
References
1. Roxby AC, Greninger AL, Hatfield KM, Lynch JB, Dellit TH, James A, et al. Detection of SARS-CoV-2 Among
Residents and Staff Members of an Independent and Assisted Living Community for Older Adults - Seattle,
Washington, 2020. MMWR Morb Mortal Wkly Rep. 2020 Apr 10;69(14):416-8.
2. European Centre for Disease Prevention and Control. Rapid Risk Assessment: Coronavirus disease 2019
(COVID-19) in the EU/EEA and the UK– ninth update Stockholm: ECDC; 2020 [updated 24 April 2020].
Available from:
https://www.ecdc.europa.eu/en/publications-data/rapid-risk-assessment-coronavirus-disease-
2019-covid-19-pandemic-ninth-update
3. Vaux S, Poujol I, Bonmarin I, Lévy-Bruhl D, Desenclos J-C. Surveillance of lower respiratory tract infections
outbreaks in nursing homes in France. European Journal of Epidemiology. 2009 2009/03/01;24(3):149-55.
4. Comas-Herrera A, Zalakain J, Litwin C, Hsu AT, Fernandez-Plotka J-L. Mortality associated with COVID-19
outbreaks in care homes: early international evidence. International Long Term Care Policy Network [21 April
2020]. Available from:
https://ltccovid.org/2020/04/12/mortality-associated-with-covid-19-outbreaks-in-care-
homes-early-international-evidence/
5. McMichael TM, Currie DW, Clark S, Pogosjans S, Kay M, Schwartz NG, et al. Epidemiology of Covid-19 in a
Long-Term Care Facility in King County, Washington. New England Journal of Medicine. 2020.
6. Gardner W, States D, Bagley N. The Coronavirus and the Risks to the Elderly in Long-Term Care. Journal of
Aging & Social Policy. 2020:1-6.
7. Arons MM, Hatfield KM, Reddy SC, Kimball A, James A, Jacobs JR, et al. Presymptomatic SARS-CoV-2
Infections and Transmission in a Skilled Nursing Facility. New England Journal of Medicine. 2020.
8. Gandhi M, Yokoe DS, Havlir DV. Asymptomatic Transmission, the Achilles’ Heel of Current Strategies to
Control Covid-19. New England Journal of Medicine. 2020.
9. Sciensano. Coronavirus Covid-19, Overall Epidemiological Situation 2020 [18 May 2020]. Available from:
https://covid-19.sciensano.be/fr/covid-19-situation-epidemiologique
10. Santé Publique France. Infection au nouveau Coronavirus (SARS-CoV-2), COVID-19, France et Monde 2020
[11 May 2020]. Available from:
https://www.santepubliquefrance.fr/maladies-et-traumatismes/maladies-et-
infections-respiratoires/infection-a-coronavirus/articles/infection-au-nouveau-coronavirus-sars-cov-2-covid-19-
france-et-monde#block-244210.
11. Robert Koch Institut. Aktueller Lage-/Situationsbericht des RKI zu COVID-19 2020 [18 May 2020]. Available
from: https://www.rki.de/DE/Content/InfAZ/N/Neuartiges_Coronavirus/Situationsberichte/Gesamt.html
12. Health Protection Surveillance Centre. Epidemiology of COVID-19 in Ireland - daily reports, May 2020 [18 May
2020]. Available from:
https://www.hpsc.ie/a-
z/respiratory/coronavirus/novelcoronavirus/casesinireland/epidemiologyofcovid-19inireland/
13. FHI Folkehelseinstituttet. Koronavirus - temaside 2020 [11 May 2020]. Available from:
https://www.fhi.no/sv/smittsomme-sykdommer/corona/
14. rtve.es. Coronavirus: Radiografía del coronavirus en residencias de ancianos: más de 17.200 fallecidos a falta
de test generalizados 2020 [12 May 2020]. Available from:
https://www.rtve.es/noticias/20200505/radiografia-del-coronavirus-residencias-ancianos-
espana/2011609.shtml
15. Lindkvist H, Dragic M. Fler än 1.700 personer smittade på äldreboenden i Region Stockholm. Dagens Nyheter. 2020.
16. Smittskydd Stockholm. Kartläggning av covid-19 på SÄBO i Stockholms län. 2020. p.
https://www.sll.se/globalassets/bilagor-till-nyheter/2020/05/kartlaggning-av-covid-19-pa-sabo-i-stockholms-
lan.pdf
17. Edwinsson L. Coronasmitta på över 500 av landets äldreboenden. Dagens Nyheter; 2020.
18. Nikel D. Sweden Health Agency Investigates High Coronavirus Death Toll In Elderly Care Homes. Forbes; 2020.
19. Socialstyrelsen. Statistik om smittade och avlidna med covid-19 bland äldre efter boendeform. 2020 Contract
No.6.7-15552/2020.
20. Office for National Statistics. Comparison of weekly death occurrences in England and Wales: up to week
ending 1 May 2020 2020 [18 May 2020]. Available from:
https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/causesofdeath/articles/compari
sonofweeklydeathoccurrencesinenglandandwales/uptoweekending1may2020
21. Office for National Statistics. Number of deaths in care homes notified to the Care Quality Commission,
England 2020 [updated 12 May 2020]. Available from:
https://www.ons.gov.uk/peoplepopulationandcommunity/birthsdeathsandmarriages/deaths/datasets/numbero
fdeathsincarehomesnotifiedtothecarequalitycommissionengland
22. Scottish Government Riaghaltas na h-Alba gs. Coronavirus (COVID-19): daily data for Scotland 2020 [updated
17 May 2020]. Available from: https://www.gov.scot/publications/coronavirus-covid-19-daily-data-for-
scotland/
23. National Records of Scotland. Deaths involving coronavirus (COVID-19) in Scotland 2020 [18 May 2020].
Available from: https://www.nrscotland.gov.uk/covid19stats
24. CDC COVID-19 Response Team. Severe Outcomes Among Patients with Coronavirus Disease 2019 (COVID-
19) - United States, February 12-March 16, 2020. MMWR Morb Mortal Wkly Rep. 2020 Mar 27;69(12):343-6.

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
13
25. Kamp J, Wilde Mathews A. Coronavirus Deaths in U.S. Nursing, Long-Term Care Facilities Top 10,000. The
Wallstreet Journal. 2020.
26. Bowden O. Long-term care homes with the most coronavirus deaths in Canada. GlobalNews. 2020.
27. KFF KAISER FAMILY FOUNDATION. State Data and Policy Actions to Address Coronavirus 2020 [18 May 2020].
Available from: https://www.kff.org/health-costs/issue-brief/state-data-and-policy-actions-to-address-coronavirus/
28. McMichael TM, Currie DW, Clark S, Pogosjans S, Kay M, Schwartz NG, et al. Epidemiology of Covid-19 in a
Long-Term Care Facility in King County, Washington. N Engl J Med. 27 March 2020.
29. McMichael TM, Clark S, Pogosjans S, Kay M, Lewis J, Baer A, et al. COVID-19 in a Long-Term Care Facility -
King County, Washington, February 27-March 9, 2020. MMWR Morb Mortal Wkly Rep. 2020 Mar
27;69(12):339-42.
30. Kimball A, Hatfield KM, Arons M, James A, Taylor J, Spicer K, et al. Asymptomatic and Presymptomatic SARS-
CoV-2 Infections in Residents of a Long-Term Care Skilled Nursing Facility - King County, Washington, March
2020. MMWR Morb Mortal Wkly Rep. 2020 Apr 3;69(13):377-81.
31. European Centre for Disease Prevention and Control. Healthcare-associated infections in long-term care
facilities 2020 [24 April 2020]. Available from:
https://www.ecdc.europa.eu/en/healthcare-associated-
infections-long-term-care-facilities
32. European Centre for Disease Prevention and Control. Point prevalence survey of healthcare associated
infections and antimicrobial use in European long-term care facilities Stockholm: ECDC; 2014 [updated April–
May 2013]. Available from:
https://www.ecdc.europa.eu/en/publications-data/point-prevalence-survey-
healthcare-associated-infections-and-antimicrobial-use-2
33. World Health Organization. International Guidelines for Certification and Classification (coding) of COVID-19
as Cause of Death 2020 [23 April 2020]. Available from:
https://www.who.int/classifications/icd/Guidelines_Cause_of_Death_COVID-19.pdf?ua=1
34. Pan L, Mu M, Yang P, Sun Y, Wang R, Yan J, et al. Clinical Characteristics of COVID-19 Patients With
Digestive Symptoms in Hubei, China: A Descriptive, Cross-Sectional, Multicenter Study. Am J Gastroenterol.
2020 Apr 14.
35. Yang X, Yu Y, Xu J, Shu H, Xia J, Liu H, et al. Clinical course and outcomes of critically ill patients with SARS-
CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respir Med.
2020 Feb 24.

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
14
Annex
Examples of monitoring systems in European countries
Belgium
Belgium set up a specific surveillance to monitor COVID-19 in residential institutions, including nursing homes and
other long-term care facilities. The data collection in nursing homes differs from one region to another as these
facilities are regulated by the regional authority. Sciensano, the federal institute of health, however, merges,
validates and analyses the data in order to have a detailed view on the evolution of COVID-19 in the Belgian
nursing homes (n=1 542). Daily and weekly surveillance bulletins are available in Dutch & French (
https://covid-
19.sciensano.be/nl/covid-19-epidemiologische-situatie).
The data collection started on 18 March in Flanders, on 20 March in Wallonia and on 26 March 2020 in Brussels
and the German-speaking region. The number of facilities participating in the surveillance is progressively
increasing (>80% of the Belgian nursing homes at present – 5 May 2020). In Flanders and Wallonia, nursing
homes daily report aggregated numbers using the region’s own surveillance system. Nursing homes in Brussels
and in the German-speaking region daily complete an online survey tool, set up by Sciensano. In addition, all
COVID-19 related outbreaks mandatorily have to be reported to the regional authorities.
The collected data include:
• Total number and number of new (i.e. since the last reporting) possible or confirmed COVID-19 cases
among residents.
• Total number and number of new (i.e. since the last reporting) possible or confirmed deaths due to COVID-
19 among residents.
• Total number and number of new (i.e. since the last reporting) possible or confirmed COVID-19 cases
among nursing home staff members.
A confirmed case of a COVID-19 infection is a person with laboratory confirmation of the virus causing COVID-19
infection, irrespective of clinical signs and symptoms. A possible COVID-19 case* is defined as a person with
signs/symptoms of an upper or lower respiratory tract infection which are new or acutely worse (in case of chronic
respiratory symptoms) OR (b) any person whose laboratory test is negative but who is diagnosed with COVID-19
based on a suggestive clinical presentation and a compatible CT thorax.
*Definition has been subject to change.
In collaboration with the regions, Sciensano aims in the near future to follow up on the characteristics of all
deceased residents since 12 March - i.e. date of birth, date of death, gender, possible, confirmed or non COVID-19
related death, method of diagnosis (if applicable) and place of death (the nursing home itself, hospital or other).
At the end of March 2020, Belgium set up a COVID-19 testing task force. The objective of this taskforce is to
significantly increase Belgian test capacity. In a first phase, test kits were sent to nursing homes in order to have a
clear picture of spread of the virus among residents and/or staff members. The ultimate goal is to expand the
testing to other healthcare sectors.
France
In France, a surveillance system of outbreaks of acute respiratory infections in long-term care facilities (LTCF) has
been in place for over 10 years. Its primary objective is to allow early and optimal management of such outbreaks
by the Regional Health Agencies (RHA) but it is also used by Santé publique France at regional and national level
to assess in real time the impact of influenza epidemics on the elderly. LTCFs (mainly those for the elderly) report
any outbreak of ARI in a timely manner (minimum of 5 ARI cases within 4 days).
This questionnaire has two sections: the first is filled out when the episode is reported to the RHA, and the second
is filled out when the episode is considered as over. Since October 2019, LTCFs complete both questionnaires on
an online platform.
Based on the data collected throughout the influenza season, the dynamic of weekly number of episodes (including
those for which influenza has been detected), the attack rate, the case-fatality rate and the influenza vaccine
coverage among the residents and the personnel can be analysed.
This surveillance is coordinated at regional level. Although probably far from comprehensive, with significant
variations between regions, it has proven to be very informative on the burden of influenza on the elderly,
particularly during the seasons with significant circulation of A(H3N2) viruses.
In the context of COVID-19, this system has been adapted to monitor the epidemic in LTCF:
• all types of LTCFs, including those for young adults/children and persons with disabilities, report at least
one case of COVID-19, probable or confirmed, immediately upon detection, using an initial electronic
reporting form on a new dedicated national online platform;
• Subsequently, LTCFs report the total number of cases and deaths, among residents and number of
cases among personnel in an aggregated manner on a daily basis. A form with the final number of cases
and deaths is completed when the episode is over;

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
15
• Local public health authorities have access to this information daily to implement control measures. Daily
and weekly reports are produced at the national and regional level.
The protocol and the questionnaires (in French) can be accessed here:
https://www.santepubliquefrance.fr/maladies-et-traumatismes/maladies-et-infections-respiratoires/infection-a-
coronavirus/articles/infection-au-nouveau-coronavirus-sars-cov-2-covid-19-france-et-monde
The weekly reports are available here: https://www.santepubliquefrance.fr/
Germany
According to the German infection protection act, the reporting of suspected and confirmed COVID-19-cases and
deaths as well as outbreaks is mandatory (via the local health authorities to the regional and national level). A local
syndromic surveillance on a daily basis (inhabitants and staff) in LTCFs has been recommended by the Robert
Koch-Institute. Within the frame of facility-based syndromic surveillance, individual details of the monitoring of the
cases, staff and visitors, test outcomes and course of the disease in the individuals should be registered. Also
measures taken in the facilities and reporting to health authorities should be documented.
Recommendations are available in German:
https://www.rki.de/DE/Content/InfAZ/N/Neuartiges_Coronavirus/Alten_Pflegeeinrichtung_Empfehlung.html
A large repository of documents to collect data from residents, staff and visitors is available from here:
https://www.rki.de/DE/Content/InfAZ/N/Neuartiges_Coronavirus/Pflege/Dokumente.html
Ireland
In Ireland, all infectious disease outbreaks are notifiable and a national surveillance system for monitoring all
infectious disease outbreaks has been in place for 15+ years. COVID-19 was made notifiable and therefore
regional Departments of Public Health notify all COVID-19 outbreaks. These outbreaks are currently notified on the
Irish national infectious disease reporting system, which is a national online repository of laboratory and
clinical/surveillance infectious disease notifiable data. This system is called CIDR - Computerised Infectious Disease
Reporting System, which includes both case based data and a facility to notify outbreaks and link all relevant cases
to these outbreaks. This system includes outbreaks in all settings – family, travel related, hospitals, LTCFs. As all
outbreaks are notifiable, there is data on both suspect and confirmed COVID-19 outbreaks in LTCFs and also on
any other outbreak in a LTCF that is notified available.
A flow chart on COVID-19 Interim assessment, testing and outbreak guidance for residents and staff in residential
facilities and LTCFs is available here. Interim Public Health and Infection Prevention Control Guidelines on the
Prevention and Management of COVID-19 Cases and Outbreaks in Residential Care Facilities and Similar Units are
available here:
https://www.hpsc.ie/a-
z/respiratory/coronavirus/novelcoronavirus/guidance/outbreakmanagementguidance/Preliminary%20RCF%20guida
nce%20document.pdf
Norway
There is mandatory reporting of all outbreaks in LTCFs to the NIPH and the local municipality public health officer
in place. Under-reporting of this system has been observed, which is also the case during the current pandemic.
The reporting is made through an online database system.
United Kingdom
England: COVID-19: guidance for supported living and home care
https://www.gov.uk/government/publications/covid-19-residential-care-supported-living-and-home-care-guidance
Public Health England: Guidelines on the management of outbreaks of influenza-like illness in care homes:
https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/747543/Influen
za-like_illness_in_care_home_2018_FINAL.pdf
Scotland: COVID-19 - Information and guidance for care home settings https://www.hps.scot.nhs.uk/web-
resources-container/covid-19-information-and-guidance-for-care-home-settings/
Coronavirus (COVID-19): clinical guidance for nursing home and residential care residents - updated May 15
https://www.gov.scot/publications/coronavirus-covid-19-clinical-and-practice-guidance-for-adult-care-homes/
Northern Ireland: COVID-19: Guidance for Nursing and Residential Care Homes in Northern Ireland:
https://www.health-ni.gov.uk/publications/covid-19-guidance-nursing-and-residential-care-homes-northern-ireland
US CDC guidelines:
https://www.cdc.gov/coronavirus/2019-ncov/hcp/nursing-homes-responding.html
https://www.cdc.gov/coronavirus/2019-ncov/hcp/nursing-homes-testing.html

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
16
Data from HALT on long-term care facilities
Table A1. Number of long-term care facilities by facility type and long-term care facility beds, by
country (2010–2017)
Country Data source
Number of LTCFs
Number of LTCF
beds
General nursing
homes
Residential
homes
'Mixed LTCFs' Total
Austria
HALT
NA
NA
817
817
72 602
Belgium
HALT-3
1 230
329
NA
1 559
146 462
Bulgaria
HALT
NA
NA
33
33
486
Croatia
HALT-3
155
170
ND
325
37 249
Cyprus
HALT-3
ND
43
47
90
3 436
Czech Republic
HALT-2
73
ND
ND
73
17 204
Denmark*
HALT-3
*
*
827
827
42 668
Estonia
HALT-3
59
NA
NA
59
1 849
Finland
HALT-3
350
1 578
NA
1 928
50 373
France
HALT-3
7 428
2 316
NA
9 744
687 936
Germany*
HALT-3
*
*
10 389
10 389
852 849
Greece
HALT-3
NA
NA
263
263
10 849
Hungary
HALT-2
1 067
110
ND
1 177
57 929
Iceland
Eurostat (2015)
ND
ND
ND
43
2 628
Ireland*
HALT-3
*
NA
578
578
30 531
Italy
HALT-3
3 219
NA
ND
3 219
186 872
Latvia
HALT-2
NA
NA
82
82
5 798
Liechtenstein
ND
ND
ND
ND
ND
ND
Lithuania*
HALT-3
*
*
154
154
11 722
Luxemburg
HALT-3
51
11
NA
62
6 966
Malta
HALT-3
NA
35
6
41
5 035
Netherlands
HALT-3
NA
NA
700
700
92 000
Norway*
HALT-3
*
*
907
907
39 583
Poland
HALT-3
257
116
NA
373
17 291
Portugal**
Ministry of
Labour,
Solidarity and
Social Security
2 445
287
337
3 069
109 740
Romania
Eurostat (2015)
ND
ND
ND
628
37 727
Slovakia
HALT-3
99
300
278
677
27 497
Slovenia
HALT-2
NA
NA
90
90
20 777
Spain*
HALT-3
*
*
5 387
5 387
372 306
Sweden*
HALT-3
*
*
2 300
2 300
93 000
UK
HALT-2/3
4 953
13 510
1 123
19 586
546 974
UK-England
HALT-2
4 684
12 789
ND
17 473
468 658
UK-N. Ireland
HALT-3
NA
195
250
445
15 924
UK-Scotland*
HALT-3
*
*
873
873
37 746
UK-Wales
HALT-3
269
526
ND
795
24 646
EU/EEA + UK
NA
26 674
16 940
16 159
62 471
3 486 999
Key:
LTCFs — long-term care facilities, the definition of LTCFs and LTCF types is provided on the ECDC protocols for surveillance of
healthcare-associated infections in LTCFs (URL:
https://www.ecdc.europa.eu/en/infectious-diseases-public-health/healthcare-
associated-infections-long-term-care-facilities);
* Country unable to make a distinction between LTCF types;
** Data source:
official data from the Strategy and Planning Office of the Ministry of Labour, Solidarity and Social Security on the
National Network of Social Services and Social Facilities http://www.cartasocial.pt/
NA — not applicable, i.e. the LTCF type is not present in the country;
ND — no data available;
NP — no participation; HALT/HALT-2/HALT-3 — ECDC Point Prevalence Survey of Healthcare-Associated Infections and Antimicrobial Use in European
Long-Term Care Facilities, 2010/2013/2016—2017 (URL: https://www.ecdc.europa.eu/en/healthcare-associated-infections-long-term-care-facilities
)

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
17
Table A2. Number of long-term care facilities (LTCFs) and population, by country
Country
LTCFs*
Population (2020)**
Population
≥80
yrs/LTCF
bed
Number
Number of
beds
Mean
size
(beds)
≥65yrs
≥80yrs
All ages
N % N % N
Austria
817
72 602
89
1 668 559
18.8
442 517
5.0
8 858 775
6.1
Belgium
1 559
146 462
94
2 165 459
18.9
646 969
5.6
11 455 519
4.4
Bulgaria
33
486
15
1 493 119
21.3
338 610
4.8
7 000 039
696.7
Croatia
325
37 249
115
838 599
20.6
217 633
5.3
4 076 246
5.8
Cyprus
90
3 436
38
141 112
16.1
32 013
3.7
875 899
9.3
Czech Republic
73
17 204
236
2 086 617
19.6
432 907
4.1
10 649 800
25.2
Denmark
827
42 668
52
1 136 063
19.6
263 746
4.5
5 806 081
6.2
Estonia
59
1 849
31
261 848
19.8
74 717
5.6
1 324 820
40.4
Finland
1 928
50 373
26
1 204 837
21.8
302 710
5.5
5 517 919
6.0
France
9 744
687 936
71
13 470 073
20.1
4 106 665
6.1
67 012 883
6.0
Germany
10 389
852 849
82
17 883 532
21.5
5 389 106
6.5
83 019 213
6.3
Greece
263
10 849
41
2 363 273
22.0
760 434
7.1
10 724 599
70.1
Hungary
1 177
57 929
49
1 889 959
19.3
433 033
4.4
9 772 756
7.5
Iceland
43
2 628
61
50 739
14.2
12 478
3.5
356 991
4.7
Ireland
578
30 531
53
691 439
14.1
163 824
3.3
4 904 240
5.4
Italy
3 219
186 872
58
13 783 580
22.8
4 330 074
7.2
60 359 546
23.2
Latvia
82
5 798
71
388 979
20.3
107 513
5.6
1 919 968
18.5
Liechtenstein
ND
ND
ND
6 861
17.9
1 456
3.8
38 378
ND
Lithuania
154
11 722
76
552 373
19.8
161 539
5.8
2 794 184
13.8
Luxemburg
62
6 966
112
88 328
14.4
24 282
4.0
613 894
3.5
Malta
41
5 035
123
92 180
18.7
20 846
4.2
493 559
4.1
Netherlands
700
92 000
131
3 314 004
19.2
798 820
4.6
17 282 163
8.7
Norway
907
39 583
44
918 841
17.2
225 999
4.2
5 328 212
5.7
Poland
373
17 291
46
6 706 044
17.7
1 660 376
4.4
37 972 812
96.0
Portugal***
3 069
109 740
23
2 244 225
21.8
661 456
6.4
10 276 617
6.0
Romania
628
37 727
60
3 596 357
18.5
906 398
4.7
19 414 458
24.0
Slovakia
677
27 497
41
874 319
16.0
179 513
3.3
5 450 421
6.5
Slovenia
90
20 777
231
413 054
19.8
111 033
5.3
2 080 908
5.3
Spain
5 387
372 306
69
9 105 575
19.4
2 880 884
6.1
46 937 060
7.7
Sweden
2 300
93 000
40
2 035 711
19.9
522 133
5.1
10 230 185
5.6
UK
19 586
546 974
28
12 272 378
18.4
3 319 956
5.0
66 647 112
6.1
UK-England**
17 473
468 658
27
10179253
18.2
2768734
4.9
55 977 178
5.9
UK-N. Ireland**
445
15 924
36
651993
20.8
170459
5.4
3 138 631
10.7
UK-Scotland**
873
37 746
43
1026114
18.9
263634
4.8
5 438 100
7.0
UK-Wales**
795
24 646
31
308197
16.4
79128
4.2
1 881 641
3.2
EU/EEA+UK
62 471
3 486 999
56
103 738 037
20.0
29 529 640
5.7
519 195 257
8.5
Key:
LTCFs — long-term care facilities, i.e. the total general nursing homes, residential homes and ‘mixed facilities’, as defined in
ECDC protocols for surveillance of healthcare-associated infections in LTCFs (URL:
https://www.ecdc.europa.eu/en/infectious-
diseases-public-health/healthcare-associated-infections-long-term-care-facilities).
* Data source: the most recent data provided by countries for an ECDC Point Prevalence Survey of Healthcare-Associated
Infections and Antimicrobial Use in European Long-Term Care Facilities, i.e. in 2016-2017, 2013 or 2010; except for Iceland and
Romania, which are Eurostat data for 2015 (see Table A1).
** all population data are Eurostat data for 2020, except for the four UK administrations, which are mid-2018 population
estimates from the UK Office for National
Statistics.(
https://www.ons.gov.uk/peoplepopulationandcommunity/populationandmigration/populationestimates/datasets/popula
tionestimatesforukenglandandwalesscotlandandnorthernireland ).
***
Data Source: official data from the Strategy and Planning Office of the Ministry of Labour, Solidarity and Social Security on
the National Network of Social Services and Social Facilities http://www.cartasocial.pt/
ND — no data available.

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
18
Suggestions for data collection and reporting forms
Table A3. Example line list to collect case data at LTCFs for internal use in the facilities
Resident details Resident location Symptoms Lab tests Case data Measures
Name
Date of birth
Sex
Primary/ lead care
provider
Room code
Floor/ unit code
Building code
Moved to (room/
floor/ building
)
Symptoms
Date of symptom
onset
Sample date
Lab result
Date lab result
received
Case status
Admission to
hospital
Date of hospital
admission
Date of recovery/
discharge/death
Outcome
Isolation in single
room
Cohorting
Face masks worn
by staff
free text
YYYY.MM.DD
M: male
F: female
U: unknown
free text
free text
free text
free text
free text
Y/N/U
YYYY.MM.DD
YYYY.MM.DD
NO TEST,
POS,
NEG,
UNK
YYYY.MM.DD
POSS: Possible,
PROB: Probable,
CON: Confirmed,
UNK: Unknown
Y/N/U
YYYY.MM.DD
YYYY.MM.DD
A: alive,
D: deceased
Y/N/U
Y/N/U
NONE: no masks
available,
MA: mask available
(type not specified)
,
SMM: Self
-made
masks,
SM: Surgical mask
s,
RES: FFP2/3
respirators,
COM: Combination
of the above
Face masks are considered the most important, particularly as source control for staff.

TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
19
Table A4. Initial data for LTCFs to report to local and national authorities with their first report (can
be updated monthly/quarterly)
Category Description Variable Data format
Date Reporting period
Date from YYYY.MM.DD
Date to YYYY.MM.DD
Location data Address
(free text, e.g. address)
LTCF
Characteristics
LTCF identifier
(Number or free text)
LTCF type (report once)
� Residential home
� Nursing home
� Mixed facility
� Palliative care
� Rehabilitation centre
� LTCF for physically or mentally
disabled
� Psychiatric LTCF
� Other LTCF type
LTCF organisation
� Public
� Private
� Non-government social care facility
� Other LTCF type
Regional code E.g. NUTS1/2 code (text)
Denominator
Residents
Total number of resident beds* N
Total number of residents N
Staff Total number of staff N
PPE**
Do staff with direct contact with residents
wear face masks?
� YES for all residents
� YES for COVID-19 cases only
� YES for all symptomatic residents
� NO face masks
� Unknown
Specify type of face mask used by staff
� No mask available
� Mask available (type unspecified)
� Self-made masks
� Surgical mask
� FFP2/3 respirators
� Combination of the above
Do visitors of residents wear face masks?
� YES all visitors
� ONLY selected visitors
� NO face masks
� Unknown
Specify type of face mask used by visitors
� No mask available
� Mask available (type unspecified)
� Self-made masks
� Surgical mask
� FFP2/3 respirators
� Combination of the above
N — number
* The total number of resident beds in the LTCF, both occupied and unoccupied beds. Beds shared by partners should be
counted as two beds.
**
Face masks are considered most important, particularly as source control for staff, other PPE can be added.
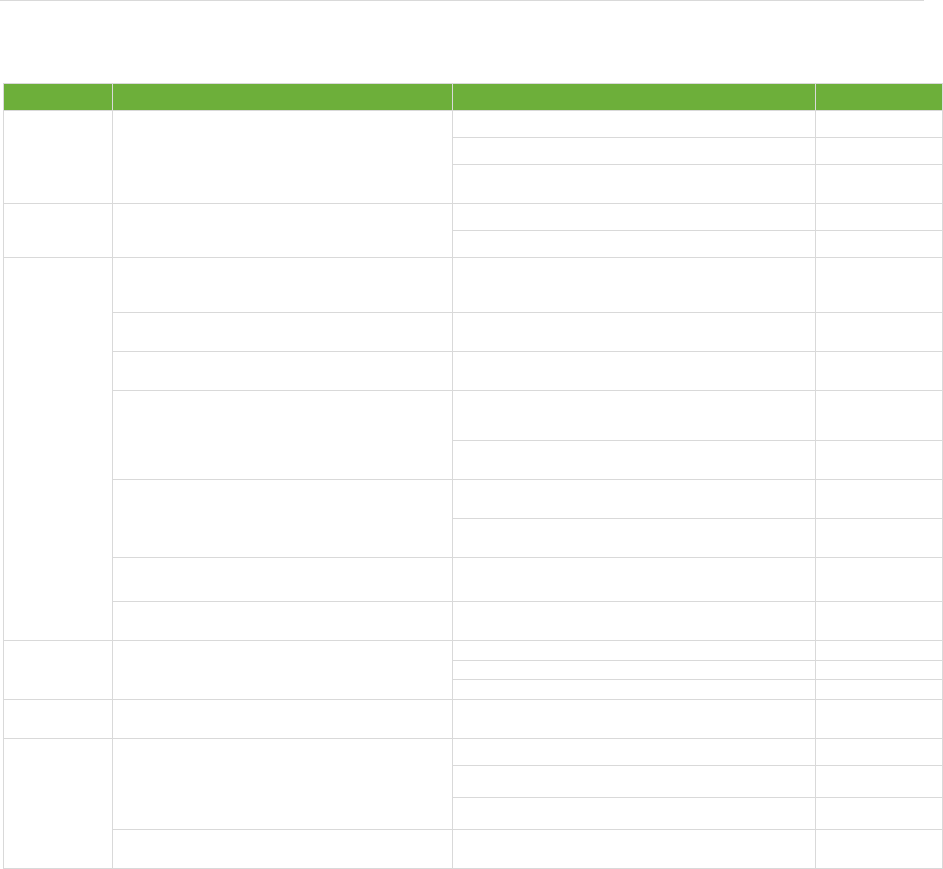
TECHINCAL GUIDANCE Surveillance of COVID-19 at long-term care facilities in the EU/EEA
20
Table A5. Data, for collection by each LTCF on a daily or weekly basis*
Category
Description
Variable
Data format
Date Reporting period
Date from
YYYY.MM.DD
Date to
YYYY.MM.DD
Start date for cumulative data (default =
2020.03.01)
YYYY.MM.DD
LTCF Characteristics
LTCF identifier
N
Location code, e.g. NUTS1/2 code
(text)
Residents
Denominator (on the day when the outbreak
is first notified)
Total residents
N
Total N of COVID-19 cases**
Cumulative cases since 1 March 2020 –or
selected date
N
Possible and probable cases
Cumulative cases since 1 March 2020 –or
selected date
N
Confirmed cases***
Cumulative symptomatic cases since 1 March
2020 –or selected date
N
Cumulative asymptomatic cases since 1 March
2020 –or selected date
N
Deaths (all causes)
Cumulative deaths in hospitals since 1 March
2020 –or selected date
N
Cumulative deaths in LTCF since 1 March 2020
–or selected date
N
Deaths among possible and probable cases
Cumulative deaths since 1 March 2020 –or
selected date
N
Deaths among confirmed cases
Cumulative deaths since 1 March 2020 –or
selected date
N
Staff
Cumulative number since 1 March 2020 – or
selected date
N of symptomatic confirmed cases
N
N of asymptomatic confirmed cases
N
N of deaths of confirmed cases
N
Residents +
Staff
Cumulative number of confirmed cases since
1 March 2020 – or selected date
N of all confirmed cases
N
Tests
For the time period included in this report
N of residents tested
N
N of staff tested
N
N of all tests
¥
N
Cumulative number since 1 March 2020 – or
selected date
N of all tests
¥
N
N — number; selected date: e.g. introduction of the virus into the country
Staff: the definition of persons as ‘staff’ should be determined at national level and should include those who work full time, part
time, or periodically; including paid and unpaid staff. Examples of staff types include but are not limited to nursing staff,
paramedical staff, recreation support team, staff concerned with cleaning, maintenance or quality control and LTCF managers
and administrative staff, including staff who only have contact with other staff members.
* LTCF is in an affected area: reporting should be daily if there is ≥1 confirmed case, daily (weekly)if there is ≥1 possible case;
LTCF is in an unaffected area: weekly or monthly if there are no cases or ≥1 possible case.
**Total number of all possible, probable, and confirmed COVID-19 cases according to ECDC case definition or defined nationally
*** If no data is available on whether a confirmed case is symptomatic or asymptomatic, assume that all confirmed cases are
symptomatic.
¥
- number of tests rather than number of people tested
